hemorrhoids
*Please scroll down for more information, tips, and videos
* Hemorrite for sale, dial 711-4141 local 297 or 254-1111 local 256 for more information
What are hemorrhoids?
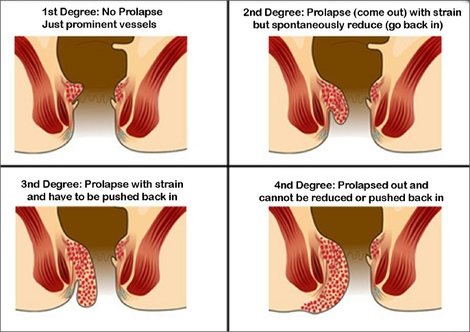
Hemorrhoids (also called piles) are swollen blood vessels in the anus and rectum that become engorged from increased pressure, similar to what occurs in varicose veins in the legs. Hemorrhoids can either be internal (inside the anus) or external (under the skin around the anus). Hemorrhoids are the most common cause of minor rectal bleeding, and are typically not associated with pain. Bleeding from hemorrhoids is usually associated with bowel movements, or it may also stain the toilet paper with blood. The exact cause of bleeding from hemorrhoids is not known, but it often seems to be related to constipation, diarrhea, sitting or standing for long periods, obesity heavy lifting and pregnancy. Symptoms from hemorrhoids may run in some families. Hemorrhoids are also more common as we get older. Fortunately, this very common condition does not lead to cancer.
How are hemorrhoids treated?
Medical treatment of hemorrhoids includes treatment of any underlying constipation, taking warm baths and applying an over-the-counter cream or suppository that may contain hydrocortisone. If medical treatment fails there are a number of ways to reduce the size or eliminate internal hemorrhoids. Each method varies in its success rate, risks and recovery time. Your doctor will discuss these options with you.
Rubber band ligation is the most common outpatient procedure for hemorrhoids in the United States. It involves placing rubber bands around the base of an internal hemorrhoid to cut off its blood supply. This causes the hemorrhoid to shrink, and in a few days both the hemorrhoid and the rubber band fall off during a bowel movement. Possible complications include pain, bleeding and infection. After band ligation, your doctor may prescribe medications, including pain medication and stool softeners, before sending you home. Contact your doctor immediately if you notice severe pain, fever or significant rectal bleeding. Surgery to remove hemorrhoids may be required in severe cases or if symptoms persist despite rubber band ligation, coagulation or sclerotherapy.
* Hemorrite for sale, dial 711-4141 local 297 or 254-1111 local 256 for more information
What are hemorrhoids?
Hemorrhoids (also called piles) are swollen blood vessels in the anus and rectum that become engorged from increased pressure, similar to what occurs in varicose veins in the legs. Hemorrhoids can either be internal (inside the anus) or external (under the skin around the anus). Hemorrhoids are the most common cause of minor rectal bleeding, and are typically not associated with pain. Bleeding from hemorrhoids is usually associated with bowel movements, or it may also stain the toilet paper with blood. The exact cause of bleeding from hemorrhoids is not known, but it often seems to be related to constipation, diarrhea, sitting or standing for long periods, obesity heavy lifting and pregnancy. Symptoms from hemorrhoids may run in some families. Hemorrhoids are also more common as we get older. Fortunately, this very common condition does not lead to cancer.
How are hemorrhoids treated?
Medical treatment of hemorrhoids includes treatment of any underlying constipation, taking warm baths and applying an over-the-counter cream or suppository that may contain hydrocortisone. If medical treatment fails there are a number of ways to reduce the size or eliminate internal hemorrhoids. Each method varies in its success rate, risks and recovery time. Your doctor will discuss these options with you.
Rubber band ligation is the most common outpatient procedure for hemorrhoids in the United States. It involves placing rubber bands around the base of an internal hemorrhoid to cut off its blood supply. This causes the hemorrhoid to shrink, and in a few days both the hemorrhoid and the rubber band fall off during a bowel movement. Possible complications include pain, bleeding and infection. After band ligation, your doctor may prescribe medications, including pain medication and stool softeners, before sending you home. Contact your doctor immediately if you notice severe pain, fever or significant rectal bleeding. Surgery to remove hemorrhoids may be required in severe cases or if symptoms persist despite rubber band ligation, coagulation or sclerotherapy.
External haemorrhoid (sometimes called a perianal haematoma)
This is less common than internal haemorrhoids. An external haemorrhoid is a small lump that develops on the outside edge of the anus. Many do not cause symptoms. However, if a blood clot forms in the haemorrhoid ('thrombosed external haemorrhoid') it can suddenly become very painful and need urgent treatment.The pain due to a thrombosed external haemorrhoid usually peaks after 48-72hours, and then gradually goes away over 7-10 days. A thrombosed external haemorrhoid may bleed a little for a few days. It then gradually shrinks to become a skin tag.
This is less common than internal haemorrhoids. An external haemorrhoid is a small lump that develops on the outside edge of the anus. Many do not cause symptoms. However, if a blood clot forms in the haemorrhoid ('thrombosed external haemorrhoid') it can suddenly become very painful and need urgent treatment.The pain due to a thrombosed external haemorrhoid usually peaks after 48-72hours, and then gradually goes away over 7-10 days. A thrombosed external haemorrhoid may bleed a little for a few days. It then gradually shrinks to become a skin tag.
|
What is the treatment for haemorrhoids?
Avoid constipation and straining at the toilet. Keep the faeces (sometimes called stools or motions) soft, and don't strain on the toilet. You can do this by the following: •Eat plenty of fibre such as fruit, vegetables, cereals, wholemeal bread, etc. •Have lots to drink.Adults should aim to drink at least two litres (10-12 cups)per day. You will pass much of the fluid as urine, but some is passed out in the gut and softens faeces. Most sorts of drink will do, but alcoholic drinks can be dehydrating and may not be so good. •Fibre supplements.If a high fibre diet is not helping, you can take bran or other fibre supplements ('bulking agents') such as ispaghula, methylcellulose or sterculia. |
•Avoid painkillers that contain codeine such as co-codamol, as they are a common cause of constipation.
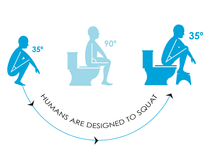
•Toileting.Go to the toilet as soon as possible after feeling the need. Some people suppress this feeling and plan to go to the toilet later. This may result in bigger and harder faeces forming which are then more difficult to pass. Do not strain on the toilet. Haemorrhoids may cause a feeling of 'fullness' in the rectum and it is tempting to strain at the end to try and empty the rectum further. Resist this. Do not spend too long on the toilet which may encourage you to strain. (For example, do not read whilst on the toilet.)The above measures will often ease symptoms such as bleeding and
•Toileting.Go to the toilet as soon as possible after feeling the need. Some people suppress this feeling and plan to go to the toilet later. This may result in bigger and harder faeces forming which are then more difficult to pass. Do not strain on the toilet. Haemorrhoids may cause a feeling of 'fullness' in the rectum and it is tempting to strain at the end to try and empty the rectum further. Resist this. Do not spend too long on the toilet which may encourage you to strain. (For example, do not read whilst on the toilet.)The above measures will often ease symptoms such as bleeding and